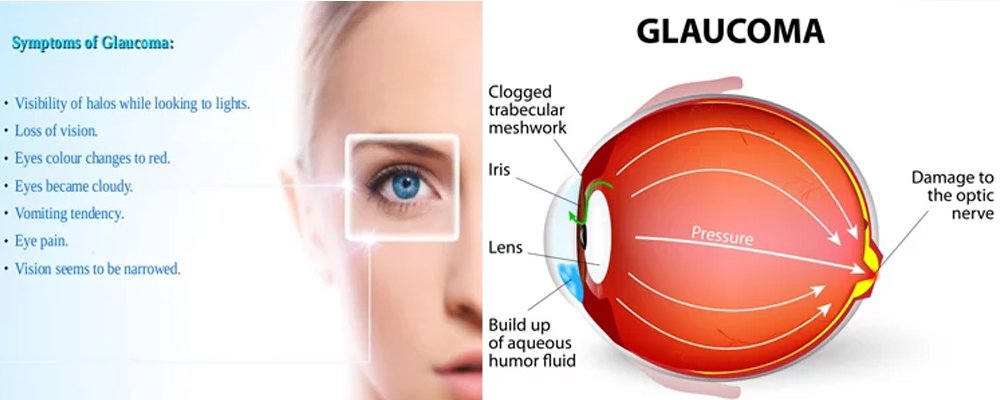
What Is Glaucoma?
The natural lens, like the cornea, makes sure that the light rays which enter the eye are properly focussed on to the retina. This results in a sharp image on the retina. The natural lens is transparent and clear which enables light to pass through it easily.
What are the Symptoms of cataract
- People over the age of 45.
- People who have a family history of glaucoma.
- People with abnormally high intraocular pressure (IOP).
- People of African descent.
- People who have: - Diabetes. - Myopia (nearsightedness).
- Regular, long-term Steroid/Cortisone use.
- A previous eye injury.
How should I know I have glaucoma?
At first, open-angle glaucoma has no symptoms. It causes no pain. Vision stays normal. Glaucoma can develop in one or both eyes.At first, open-angle glaucoma has no symptoms. It causes no pain. Vision stays normal. Glaucoma can develop in one or both eyes.
Without treatment, people with glaucoma will slowly lose their peripheral (side) vision. As glaucoma remains untreated, people may miss objects to the side and out of the corner of their eye. They seem to be looking through a tunnel. Over time, straight-ahead (central) vision may decrease until no vision remains.
Many people may know of the "air puff" test or other tests used to measure eye pressure in an eye examination. But, this test alone cannot detect glaucoma. Glaucoma is found most often during an eye examination through dilated pupils. This means drops are put into the eyes during the exam to enlarge the pupils. This allows the eye care professional to see more of the inside of the eye to check for signs of glaucoma.
Can glaucoma be cured?
No. There is no cure for glaucoma. Vision lost from the disease cannot be restored. With treatment, further visual loss can be prevented.
What are the types of glaucoma?
There are mainly 3 types of glaucoma:
1. Open angle glaucoma: About half of Americans with chronic glaucoma don't know they have it. This common type of glaucoma gradually reduces your peripheral vision without other symptoms. By the time you notice it, permanent damage already has occurred. If your IOP remains high, the destruction caused by POAG can progress until tunnel vision develops, and you will be able to see only objects that are straight ahead.
2. Closed Angle Glaucoma: Angle-closure or narrow-angle glaucoma produces sudden symptoms such as eye pain, headaches, halos around lights, dilated pupils, vision loss, red eyes, nausea and vomiting. These signs may last for a few hours, then return again for another round. Each attack takes with it part of your field of vision.
3. Secondary glaucoma. Symptoms of chronic glaucoma following an eye injury could indicate secondary glaucoma, which also may develop with presence of eye infection, inflammation, a tumor or an enlarged cataract.
- 1. The inner eye pressure
- 2. The shape and color of the optic nerve
- 3. The complete field of vision
- 4. The angle in the eye where the iris meets the cornea
- 5. Thickness of the cornea
Examining...
- 1. Tonometry
- 2. Ophthalmoscopy (dilated eye exam)
- 3. Perimetry (visual field test)
- 4. Gonioscopy
- 5. Pachymetry
Name of Test
Services Offered:
Computerised Visual Field Analysis:
A visual field test is an examination that may be performed to analyze a patient's visual field. the test consists basically of responding every time a flash of light is perceived, all the while looking straight ahead. This test can be completed anywhere from about 10-30 min depending on the patients co-operation.
Gonioscopy:
Gonioscopy is an eye examination to look at the front part of your eye (anterior chamber) between the cornea and the iris. Gonioscopy is a painless examination to see whether the area where fluid drains out of your eye (called the drainage angle) is open or closed. It is often done during a regular eye examination, depending on your age and whether you are at high risk for developing glaucoma. A special lens is placed lightly on the front of your eye, and a narrow beam of bright light is pointed into your eye. Your doctor looks through the slit lamp at the width of the drainage angle.
Cornea Thickness:
Apachymeter is a medical device used to measure the thickness of the eye's cornea. It is used to perform Corneal pachymetry and is useful in screening for patients suspected of developing glaucoma among other uses. Pachymetry can help your diagnosis, because corneal thickness has the potential to influence eye pressure readings. With this measurement, your doctor can better understand your IOP reading and develop a treatment plan that is right for you. The procedure takes only about a minute to measure both eyes.
Why Are There So Many Diagnostic Exams?
Diagnosing glaucoma is not always easy, and careful evaluation of the optic nerve continues to be essential to diagnosis and treatment. The most important concern is protecting your sight. Doctors look at many factors before making decisions about your treatment. If your condition is particularly difficult to diagnose or treat, you may be referred to a glaucoma specialist. A second opinion is always wise if you or your doctor become concerned about your diagnosis or your progress.
Treatment
State of the art MEDICAL line of management
Why Are There So Many Diagnostic Exams?
- Trabeculectomy
- Combined phacoemulsification and Trabeculectomy
- Cyclodestructive Procedures